

- Home
- Companies
- Remington Medical Inc.
- Articles
- Cost Efficiency for Single-Use vs. ...
Cost Efficiency for Single-Use vs. Reusable Medical Drainage Bag Systems
When hospitals evaluate a medical drainage bag, the conversation often begins and ends with per-unit price. But while upfront cost is an important factor, it rarely tells the full When hospitals evaluate a medical drainage bag, the conversation often begins and ends with per-unit price. But while upfront cost is an important factor, it rarely tells the full story. As healthcare systems face increasing pressure to control expenses without compromising patient safety, comparing single-use and reusable medical drainage bag options requires a broader lens. Discover both direct and indirect cost factors to make informed, defensible decisions.story. As healthcare systems face increasing pressure to control expenses without compromising patient safety, comparing single-use and reusable medical drainage bag options requires a broader lens. Discover both direct and indirect cost factors to make informed, defensible decisions.
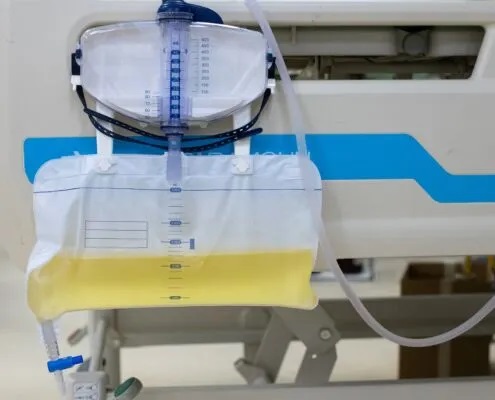
In hospitals, clinical decisions have downstream operational consequences. Selecting a medical drainage bag directly impacts staffing workflows, infection prevention strategies, and compliance requirements across departments. When these factors are not evaluated together, organizations risk optimizing for price while increasing total cost of care elsewhere.
Cost efficiency is especially critical as hospitals standardize supplies across units and care environments. A product that performs well in one setting may introduce inefficiencies in another if reprocessing capacity, staffing levels, or infection risk tolerance differ.
Evaluating both single-use and reusable options through a total cost lens allows stakeholders to align product selection with real-world usage.
At first glance, reusable medical drainage bag systems often appear more economical due to lower per-use costs over time. Once purchased, these systems can theoretically be deployed repeatedly, spreading initial investment across multiple patients. However, direct costs extend beyond the bag itself and vary significantly based on usage patterns and replacement cycles.
Single-use medical drainage bag options typically carry a higher per-unit price but eliminate the need for replacement components and ongoing maintenance. For facilities managing high patient turnover, predictable per-use pricing can simplify budgeting and inventory planning. The cost comparison becomes more nuanced when factoring in how frequently reusable components must be replaced due to wear, damage, or compliance standards.
Additionally, different types of medical drainage may require specialized configurations or accessories, which can affect direct costs for both options.
While direct costs are visible on purchase orders, operational expenses often represent a larger portion of total cost over time. These hidden costs vary widely between single-use and reusable medical drainage bag systems.
Reusable drainage systems introduce labor-intensive processes that extend well beyond bedside care. Staff must collect used bags, transport them to reprocessing areas, clean and disinfect them, inspect for damage, and prepare them for reuse. Each step consumes staff time and requires consistent execution to meet hospital infection control standards.
Labor availability and wage variability further complicate this equation. In facilities experiencing staffing shortages or high turnover, reprocessing tasks may compete with direct patient care priorities. Even small inefficiencies can accumulate when multiplied across high patient volumes, increasing operational costs in ways that are difficult to quantify upfront.
Hospitals relying on reusable systems must also maintain the infrastructure necessary to support safe reprocessing. This includes sterilization equipment, cleaning agents, documentation systems, and routine validation processes. These assets require capital investment, ongoing maintenance, and regular compliance audits.
For facilities without centralized reprocessing departments, these requirements can strain existing resources or necessitate outsourcing. Infrastructure costs are often excluded from product-level comparisons, but they play a significant role in determining the true cost-efficiency of a medical drainage bag system.
Hospital infection control remains a top priority across all care settings. And unfortunately, reusable drainage systems inherently introduce opportunities for variability in cleaning and handling processes. Even with established protocols, deviations can occur due to human error, time constraints, or inconsistent training.
Single-use medical drainage bag options reduce this variability by eliminating reprocessing steps entirely. By arriving sterile and being disposed of after use, they support standardized workflows and minimize opportunities for cross-contamination. This consistency can be especially valuable when infection risk carries significant clinical and financial consequences.
While infection-related costs are not always immediately visible, they can include extended patient stays, additional treatments, and increased reporting requirements. When viewed through a risk-management lens, the infection prevention benefits of disposables may offset higher per-unit costs in certain care environments.
Explore Remington Medical’s drainage bag options and learn how they help support efficiency, safety, and streamlined operations across a wide range of clinical settings.
Our Drainage Bags
Sustainability discussions often frame reusable products as environmentally preferable due to reduced solid waste. However, a comprehensive assessment must account for the resources consumed during reprocessing. Water usage, energy demands, chemical cleaners, and packaging all contribute to the environmental footprint of reusable medical drainage bag systems.
Disposable medical products present different sustainability challenges, primarily related to waste volume and disposal practices. Some healthcare organizations find that reduced water and energy consumption from eliminating reprocessing offsets the environmental impact of increased waste. The sustainability equation varies depending on facility infrastructure, waste management partnerships, and organizational environmental goals.
Rather than assuming one option is inherently more sustainable, hospitals benefit from evaluating environmental impact alongside operational efficiency. This balanced approach supports informed decision-making that aligns with both financial and sustainability objectives.
The cost efficiency of a medical drainage bag often depends on where and how it is used. Different hospital environments place different demands on drainage systems, influencing which option delivers the best value.
In intensive care units, where patients face higher infection risks and staff manage complex workflows, single-use systems may support consistency and risk reduction. In contrast, outpatient or lower-acuity settings with predictable usage patterns may find reusable options more feasible if reprocessing resources are readily available.
Patient volume, length of use, staffing ratios, and compliance requirements all shape the cost-efficiency equation. Evaluating these variables by department allows hospitals to align product selection with actual operational needs rather than adopting a one-size-fits-all approach.
Instead of asking whether single-use or reusable systems are universally cheaper, hospitals benefit from asking which option best supports their clinical and operational priorities. A cost-efficiency framework considers total cost of ownership, including labor, infrastructure, infection risk, and sustainability factors.
This approach encourages collaboration between clinical teams, supply chain professionals, and infection prevention leaders. By evaluating how a medical drainage bag performs within real-world workflows, stakeholders can make purchasing decisions that are easier to justify internally and more resilient over time.
As healthcare delivery models evolve, flexibility and consistency become increasingly valuable. A structured evaluation framework helps organizations adapt product choices as patient volumes, staffing levels, and regulatory expectations change.
If your team is reassessing drainage solutions or seeking to better understand the total cost implications of single-use versus reusable options, Remington Medical can help. Reach out to explore drainage bag solutions designed to support efficiency, consistency, and hospital-ready performance across care environments.
